News
Shared Care
Shared Care
Broadshires Health Centre -Shared Care Prescribing Policy (provisional)
Effective from: 01/03/2026
Reviewed monthly
1. Purpose of this Policy
Broadshires Health Centre is committed to providing safe, equitable, and sustainable care for all patients registered with the practice.
This policy sets out the practice approach to Shared Care Agreements (SCAs) for medications initiated by specialist services.
Shared care arrangements allow prescribing and monitoring responsibilities to be shared between secondary care specialists and GP practices once treatment has been initiated and stabilised.
While shared care can support continuity of care for individual patients, it requires additional clinical oversight, administrative capacity, and monitoring infrastructure within general practice.
These activities are not routinely funded within the NHS General Medical Services (GMS) contract, and practices must therefore carefully assess whether they have the resources and capacity to safely deliver shared care arrangements.
This policy ensures that shared care prescribing is undertaken only where it is clinically safe, appropriately supported by specialist services, and sustainable within available resources.
2. What is a Shared Care Agreement?
A Shared Care Agreement (SCA) is a formal arrangement between:
- The patient
- A specialist clinician (for example a hospital consultant or specialist service)
- The GP practice
Under shared care:
- The specialist retains overall clinical responsibility for the condition
- The GP practice may agree to prescribe medication and undertake monitoring
- The specialist remains responsible for treatment decisions and ongoing specialist review
Shared care agreements are voluntary and are not part of core contractual obligations for general practice.
3. Principles of Shared Care at Broadshires Health Centre
Broadshires Health Centre will consider shared care where:
- The medication has been initiated and stabilised by a specialist
- A formal written shared care protocol is provided
- The specialist service remains responsible for ongoing clinical review
- Monitoring requirements are safe and feasible within primary care
- Adequate clinical and administrative resources exist to support the arrangement
The practice has a duty to balance the needs of individual patients with the safe delivery of care for the wider practice population.
Where shared care arrangements place significant additional workload or unfunded responsibilities on general practice, the practice may decline to participate.
4. Criteria for Accepting Shared Care
Shared care will only be considered where all of the following apply:
4.1 Specialist initiation and stabilisation
The specialist must:
- Confirm the diagnosis
- Initiate the medication
- Undertake dose titration
- Ensure the patient is stable prior to requesting shared care
GPs will not initiate specialist-only medications.
4.2 Written shared care documentation
A written shared care agreement must be provided that clearly outlines:
- Diagnosis and treatment plan
- Current medication and dosage
- Monitoring requirements and frequency
- Responsibilities of the specialist, GP practice and patient
- Thresholds for abnormal results
- Process for medication adjustments
- Named responsible specialist and contact details
Requests without clear documentation may be declined.
4.3 Ongoing specialist oversight
The specialist must:
- Provide ongoing follow-up and review
- Remain responsible for treatment decisions
- Be available for advice if concerns arise
- Accept the patient back if treatment becomes unstable
If specialist oversight ceases, the practice may withdraw from the shared care arrangement.
5. Private Providers and Right to Choose
Shared care may occasionally be requested following assessment by:
- NHS Right to Choose services
- Private providers
The practice will only consider shared care where:
- The provider is appropriately qualified and regulated
- A formal shared care agreement is supplied
- The specialist remains responsible for ongoing review
- Safe monitoring arrangements are in place
Where a provider does not offer ongoing follow-up or specialist responsibility, the practice will not take over prescribing.
6. ADHD Medication – Practice Position
Broadshires Health Centre recognises that many patients are seeking assessment and treatment for ADHD, and that demand for ADHD services nationally has increased significantly.
ADHD medications require:
- Specialist diagnosis
- Careful dose titration
- Ongoing physical health monitoring (e.g. blood pressure, pulse, weight)
- Regular specialist review
- Careful governance as many medications are controlled drugs
While shared care arrangements for ADHD medication exist in some areas, there is currently no locally commissioned service or dedicated funding to support the transfer of ADHD prescribing and monitoring into general practice within Oxfordshire.
The monitoring, prescribing governance, and administrative workload associated with ADHD shared care represent a significant additional responsibility for GP practices, which is not funded within the core GP contract.
Given the current pressures on general practice and the absence of commissioned funding or resources to safely support this work, Broadshires Health Centre will not enter into new Shared Care Agreements for ADHD medication.
Responsibility for prescribing, monitoring, and medication review therefore remains with the specialist service that initiated treatment.
This applies to ADHD treatment initiated through:
- NHS specialist services
- NHS Right to Choose providers
- Private ADHD providers
Patients receiving ADHD medication should therefore contact their specialist provider for prescriptions, medication reviews, and ongoing management.
Diagnosis and treatment pathways for ADHD, including medication initiation, review, and prescribing arrangements, are commissioned and funded by the NHS Integrated Care Board (ICB) through specialist services.
Where shared care prescribing is not commissioned or funded within primary care, responsibility for prescribing and monitoring ADHD medication remains with the specialist provider responsible for the patient’s care.
GP practices are not commissioned or resourced to independently provide specialist ADHD medication management in the absence of an agreed and funded shared care pathway.
Broadshires Health Centre will therefore continue to refer patients to appropriate specialist services for ADHD assessment and treatment, but prescribing and medication review must remain under the care of the specialist service unless a locally commissioned and funded shared care service is introduced.
7. Existing Shared Care Agreements
Existing shared care arrangements may be reviewed periodically to ensure they remain safe and sustainable.
Where necessary, the practice may review or withdraw from shared care agreements if:
- Specialist follow-up is no longer provided
- Monitoring requirements cannot be safely delivered
- Practice capacity or resources change
8. Patient Responsibilities
Patients prescribed medication under shared care are expected to:
- Attend specialist follow-up appointments
- Attend monitoring appointments arranged by the GP practice
- Inform the practice of side effects or concerns
- Request prescriptions in a timely manner
Failure to complete required monitoring may result in prescribing being paused for safety reasons.
9. Review of Policy
This policy will be reviewed periodically to ensure it reflects current clinical guidance, commissioning arrangements, and practice capacity.
Approved by: Partners, Broadshires Health Centre
Date approved: 01/03/2026
Review date: 01/04/2026
Published on 13th Mar 2026
GLP-1
Update on GLP-1 Medicines for Weight Loss We’re pleased to share that NHS England has now announced national commissioning of GLP-1 medications (such as Wegovy) to support weight management. This marks a positive step forward in helping some patients manage their weight and improve their overall health. However, we want to let you know that local commissioning arrangements are not yet in place. Our Integrated Care Board (ICB) has advised us not to prescribe these medicines until local pathways are formally agreed.. Who Will Be Eligible in Year One? In this first phase, access to GLP-1 medicines will be limited to a small, high-risk group of patients who meet the strict national criteria set by NHS England. To be eligible, patients must have: 🔹 A BMI over 40 and 🔹 Four or more of the following weight-related health conditions: · Type 2 diabetes mellitus · Hypertension (high blood pressure) · Dyslipidaemia (abnormal cholesterol or lipid levels) · Obstructive sleep apnoea · Cardiovascular disease We understand that this means many patients will sadly not be eligible in the first year, even once prescribing is locally approved. What We’re Doing Whether or not you meet the Year One criteria, lifestyle changes remain key to long-term weight management. These medications work best when combined with healthy eating, physical activity, and behavioural support. Thank you for your understanding and patience as we wait for the local service to be launched. We’re committed to supporting your health and will keep you updatedGLP-1 Medicine for Weight Loss
Support While You Wait
Published on 13th Mar 2026
Total Triage
From the 1st October 2025 we are moving to a Total Triage model.
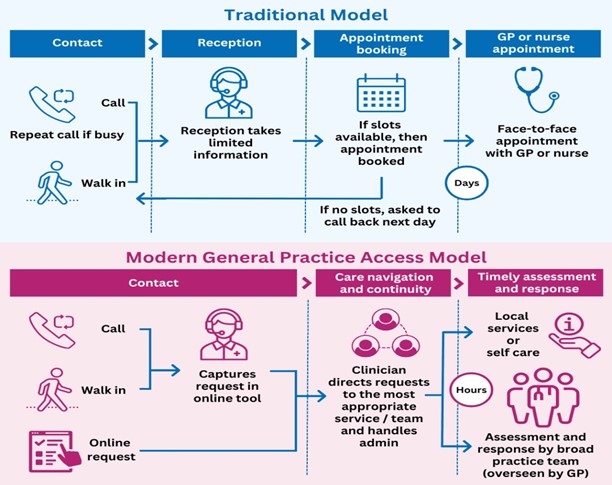
What is Total Triage?
Total triage is a General Practice workflow where every patient contacting a practice first provides some information on the reasons for contact and is triaged before making an appointment.
All patient requests will be triaged by one of our GPs who will decide what the best course of action is. Where necessary, we might ask you to answer a few additional questions to help our doctor prioritise those patients who need more urgent care.
You could be given a face to face or telephone appointment, you could have a reply from the GP with self-care advice, or you could be signposted to a more appropriate service.
The main purpose of the Total Triage model is to:
- enhance the quality of care our patients receive
- ensure they are given the most appropriate appointment or advice to meet their needs
- communicate with patients in a timely way
How does it work?
All patients need to submit their request via the surgery’s website.
Ideally, patients will submit their own request, however, we appreciate that this may not be possible for some patients. If you are unable to use or access the online form then please contact the surgery in the usual way and we will complete the request for you, which will be added to the triage list to be reviewed by the GP.
Please note that in order for the GP to triage your request in a timely manner it is very important to provide detailed and accurate information about your symptoms.
For example, if a patient has a cough, it would be much easier for the GP to triage the request with the following information: ‘I have had a cough for 10 days. I have already used over the counter medicine, but it is not helping and in the last couple of days my cough has been worsening, and it feels more chesty. I also have a high temperature.’
If the information given is less detailed, such as ‘I have a cough’, it makes it harder for the GP to triage, and we will need more information.
The Total Triage service will be open Monday to Friday. During the weekend or bank holidays please continue to use the 111 service or call 999 for life threatening emergencies.
Please note that at times we may temporarily suspend the online triage form to help manage the demand. In these circumstances you will see the following:
- a message to advise that the Patient Triage is temporarily unavailable and information on when the link will be active again and how to contact the practice another way
- a message prompting patients to use NHS 111 online, to find a local pharmacy or attend the Urgent Treatment Centre
How does this benefit you?
We know that change can be difficult sometimes, but we are confident that Total Triage will bring many benefits to our patients – for example:
- Total Triage has been shown to reduce waiting times, and it enables us to attend to your medical needs more promptly.
- Using digital communication will mean that you can engage with us from the comfort of your home or workplace.
- Clinical triage ensures that limited healthcare resources are allocated to patients who need them most urgently.
- Total Triage will address the increasing demand for appointments and reduce the frustration of having to call and be in a long queue at 8am.
If you have any questions or concerns, our team is here to guide and support you.
Thank you for supporting us with this new project.
Sincerely,
The BHC team
Published on 1st Oct 2025
Page created: 22 January 2025